May is Lyme Disease Awareness Month. An estimated 476,000 Americans are diagnosed and treated for Lyme disease each year. While Lyme disease is the most common tickborne illness in the United States, numerous other tickborne diseases occur including anaplasmosis, babesiosis, ehrlichiosis, Rocky Mountain spotted fever, and tularemia, as shown on the map below. Ticks can also cause medical conditions such as Alpha-gal syndrome, a potentially life-threatening allergy to food and consumer products derived from mammals that can develop after being bitten by a lone star tick (Amblyomma americanum).
Image
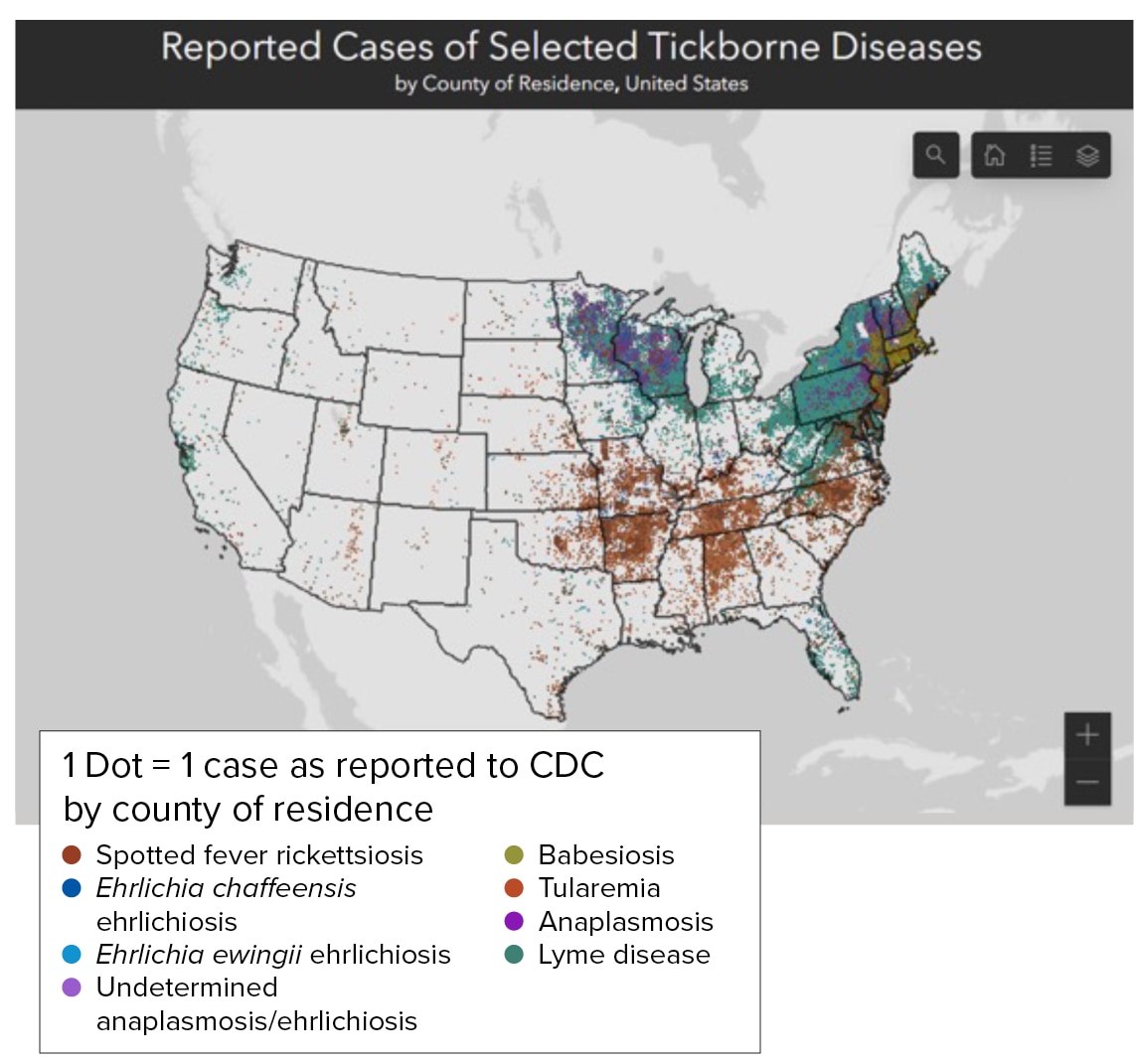
Figure: Geographic distribution of select tickborne diseases. For more information, visit the interactive map at www.cdc.gov/ticks/ data-summary/geographic-distribution.html
Risk of exposure to ticks and tickborne disease varies based on time of year, geographic location, and time spent outdoors in tick habitat. Along with deer abundance and land use patterns, climate is one of several factors that define when and where Lyme and other tickborne diseases are most likely to occur. Different climates throughout the U.S. support different species of ticks, which spread different diseases. Changing climate patterns can alter the natural environment and longstanding ecological relationships. Mild winters and warmer early spring temperatures are expanding the seasons when ticks are active, resulting in more weeks of the year that Americans are at risk of tick encounters. To track current trends on tick exposure in your region, visit the CDC website on transmission.
Outdoor workers are at increased risk of tickborne diseases if they work at sites where ticks are common. Worksites with woods, bushes, high grass, or leaf litter are likely to have more ticks. Children ages 5 to 15 years are also at increased risk of tick-borne diseases, especially if they play in tick-prone areas.
The Expanding Distribution of Lyme Disease
The geographic range of infected ticks is changing, putting an increasing number of communities at risk for Lyme and other tickborne diseases. For example, although the reported nationwide incidence of Lyme disease remained fairly stable from 2008 to 2019 at approximately 11 cases per 100,000 people per year, some states saw marked increases in incidence.
Image
Image
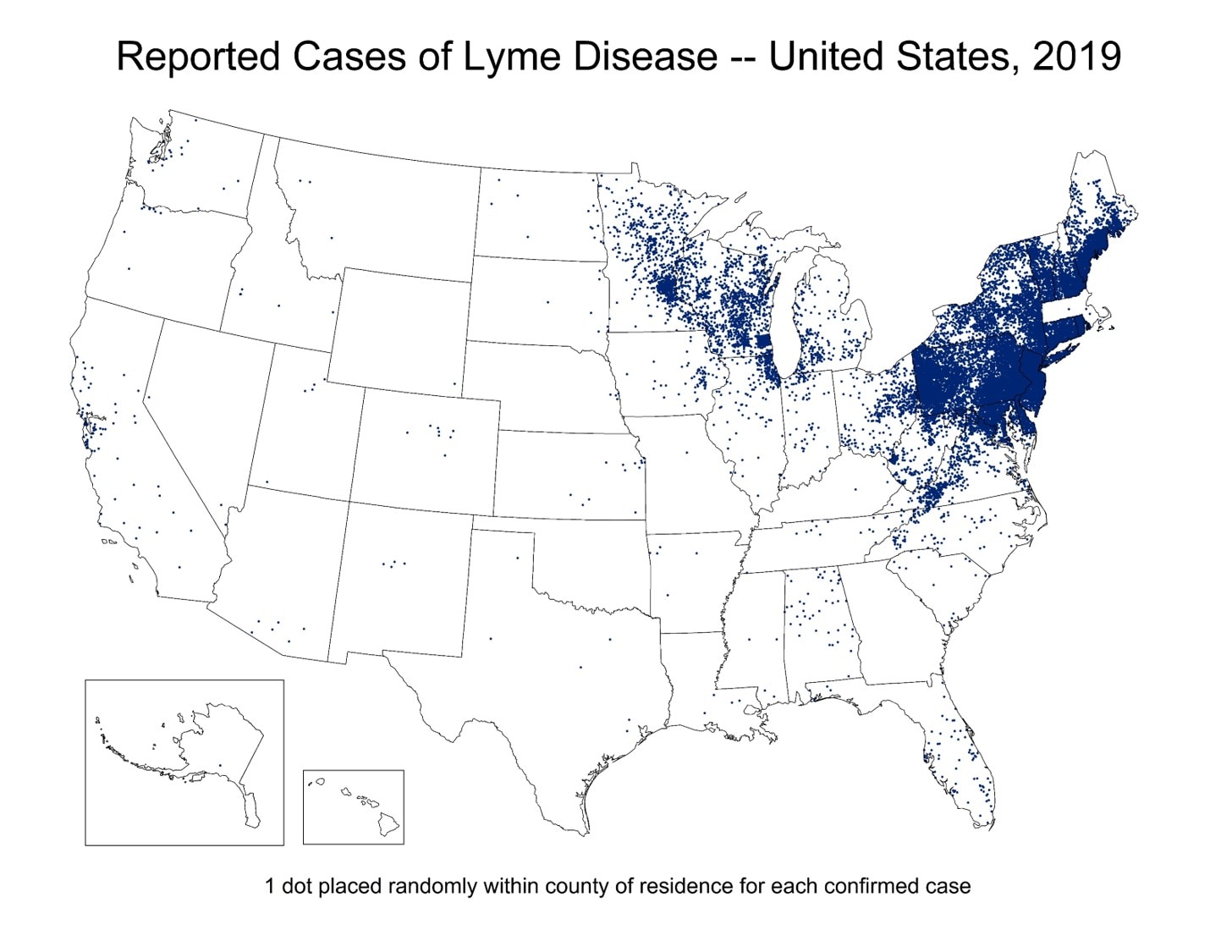
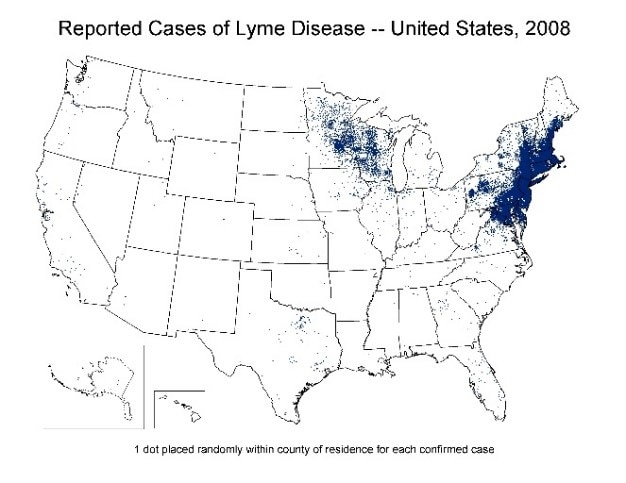
Figure: Lyme disease occurs primarily in the upper midwestern, mid-Atlantic, and northeastern United States. It is transmitted by blacklegged (deer) ticks, which also transmit the agents of anaplasmosis, babesiosis and Powassan virus disease. The lack of dots in Massachusetts in 2019 is due to a difference in reporting standards, not an absence of Lyme disease.
The greatest per capita increases in Lyme disease from 2008 to 2019 have been reported in Vermont, which had an incidence rate of 170 cases per 100,000 people in 2019 (versus 65 cases per 100,000 people in 2008); Maine, which had an incidence rate of 161 cases per 100,000 people in 2019 (versus 69 cases per 100,000 people in 2008); Rhode Island, which had an incidence rate of 92 cases per 100,000 people in 2019 (versus 20 cases per 100,000 people in 2008); Pennsylvania, which had an incidence rate of 70 cases per 100,000 people in 2019 (versus 30 cases per 100,000 people in 2008); and West Virginia, which had an incidence rate of 49 cases per 100,000 people in 2019 (versus 7 cases per 100,000 people in 2008).
How to Prevent Tick Bites and Tickborne Diseases
Avoiding tick bites is the first line of defense against Lyme and other tickborne diseases. Tick bite prevention can take place before and after spending time outside. Before you go outdoors, use Environmental Protection Agency (EPA)-registered insect repellents, treat clothing and gear with products containing 0.5% permethrin, and talk to your veterinarian about the best tick prevention products for your dog. If possible, when spending time outside, avoid wooded and brushy areas with high grass and leaf litter where ticks may live. After spending time outdoors, check your body for ticks, take a shower within 2 hours, and check your clothing, gear, and pets for ticks that may have caught a ride into your home. You may also consider using landscaping methods to prevent ticks in the yard. If you discover a tick on you or your pet, follow the recommended steps for proper tick removal as soon as possible
In areas of the eastern United States where Lyme disease is common, people are most likely to be bitten by blacklegged (deer) ticks during two times of the year: from April through July when nymphs are active, and again from September through November when adults are most active. Though people can get bitten any time ticks are present.
Image
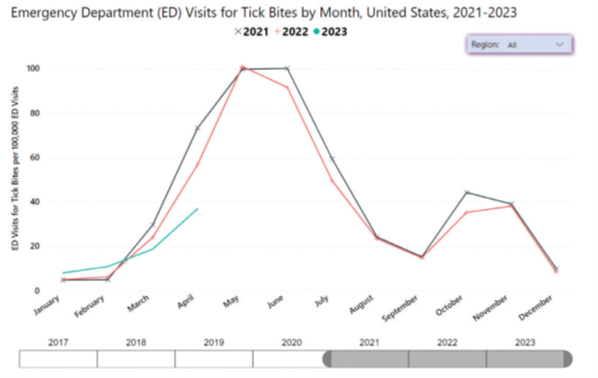
Figure: Emergency department (ED) visits for tick bites by month for 2021–2023. This graph shows 2023 following a similar pattern to previous years, with tick bites spiking in the spring. A second, smaller spike occurs in the fall when adult ticks are active. More information can be found at: www.cdc.gov/ticks/tickedvisits/index.html
Nymphal blacklegged ticks pose the greatest risk of spreading disease due to their abundance and small size (about the size of a poppy seed), which makes their detection difficult. In fact, Lyme disease patients are often not even aware of a tick bite before getting sick. Adult deer ticks are active in the spring and fall; however, due to their larger size (about the size of a sesame seed), adult ticks are more likely to be detected and removed from people before disease transmission can occur.
Image

Image source: https://www.cdc.gov/lyme/transmission/index.html
Figure: The different sizes of the blacklegged tick through 4 stages: egg, larvae, nymph, and adult.
The Centers for Disease Control and Prevention (CDC) Ticks website and Tickborne Diseases of the United States manual has information on specific tickborne diseases including information on how to avoid tick bites, common symptoms, and treatment. The Tick Bite Bot can assist you in removing attached ticks and seeking health care, if appropriate, after a tick bite. CDC has also issued guidance for clinicians on caring for patients after a tick bite. CDC has additional interactive maps displaying tick surveillance data of four tick species and surveillance of tickborne pathogens identified in blacklegged and western blacklegged ticks.
The Food and Drug Administration (FDA) has additional information on Lyme disease symptoms, treatment, and prevention for people and pets. The Environmental Protection Agency (EPA) has a tool to help find the insect repellent that is right for you.
Image
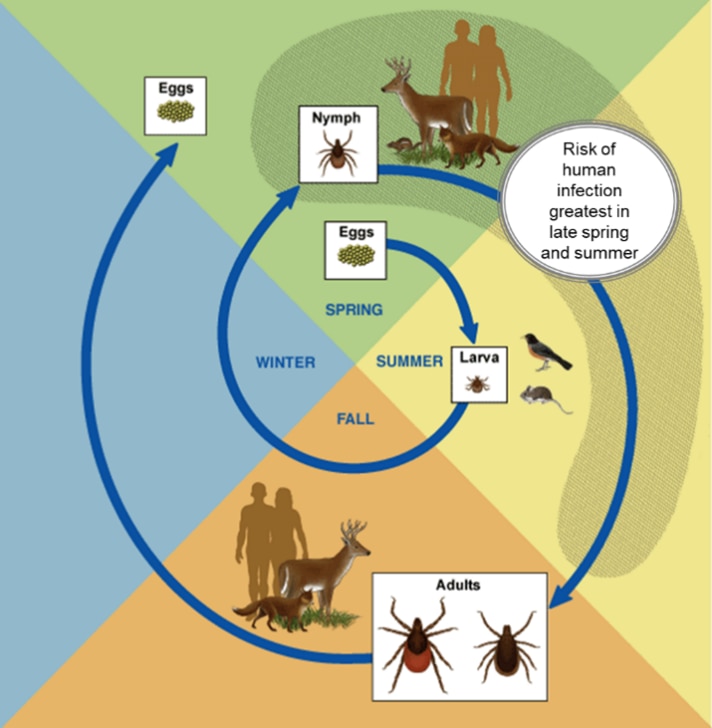
Figure: The life cycle of the blacklegged tick, Ixodes scapularis, generally lasts 2 years, during which it goes through 4 stages: egg, larvae, nymph, and adult. More information can be found at: https://www.cdc.gov/ticks/life_cycle_and_hosts.html
Alpha-gal Syndrome
Alpha-gal syndrome (AGS) is a serious, potentially life-threatening allergic condition associated with tick bites. AGS is also called alpha-gal allergy, red meat allergy, or tick bite meat allergy. AGS is not caused by an infection. Evidence suggests that AGS is primarily associated with the bite of a lone star tick (Amblyomma americanum) in the U.S., but other kinds of ticks have not been ruled out. More research is needed to understand the role ticks play in triggering AGS and why certain people develop AGS.
Image

Figure: A picture of an adult female lone star tick. Source: https://phil.cdc.gov/Details.aspx?pid=8676
People with AGS have delayed allergic reactions to a sugar molecule called alpha-gal (galactose-α-1,3-galactose), which is found in the tissues of most mammals. Alpha-gal can be found in meat such as pork, beef, rabbit, lamb, and venison, and in products made from mammals, including gelatin, cow’s milk, and milk products. Alpha-gal is not found in fish, reptiles, birds, or people.
AGS symptoms, such as hives or itchy rash, nausea or vomiting, or heartburn or indigestion, can occur 2 to 10 hours after ingestion of red meat or other products containing alpha-gal. Patients with AGS have varying tolerance and sensitivity to products containing the alpha-gal sugar, and AGS reactions can differ from person to person, ranging from mild to life-threatening. Patients with AGS who experience anaphylaxis (a potentially life-threatening reaction involving multiple organ systems) may need urgent medical care.
In the U.S., the majority of patients are adults living in the southern, mid-Atlantic, and midwestern regions. A 2023 CDC report investigating testing data showed that there were more than 110,000 suspected cases of AGS between 2010 and 2022. Additionally, suspected cases are on the rise –— from 2017 to 2021, there were approximately 15,000 new positive test results for AGS in the U.S. per year. This is likely an underestimate because the diagnosis of AGS requires a clinical exam and a positive diagnostic test, and some people may not get tested. This underestimate may also be due to a lack of healthcare provider awareness of AGS. A 2022 CDC survey of 1,500 health care providers found that only 5% felt “very confident” in their ability to diagnose or manage cases of AGS. It is possible that as many as 450,000 people might have been affected by AGS in the U.S. since 2010, but additional research and surveillance are needed to better understand how many people are affected by this condition.
Image
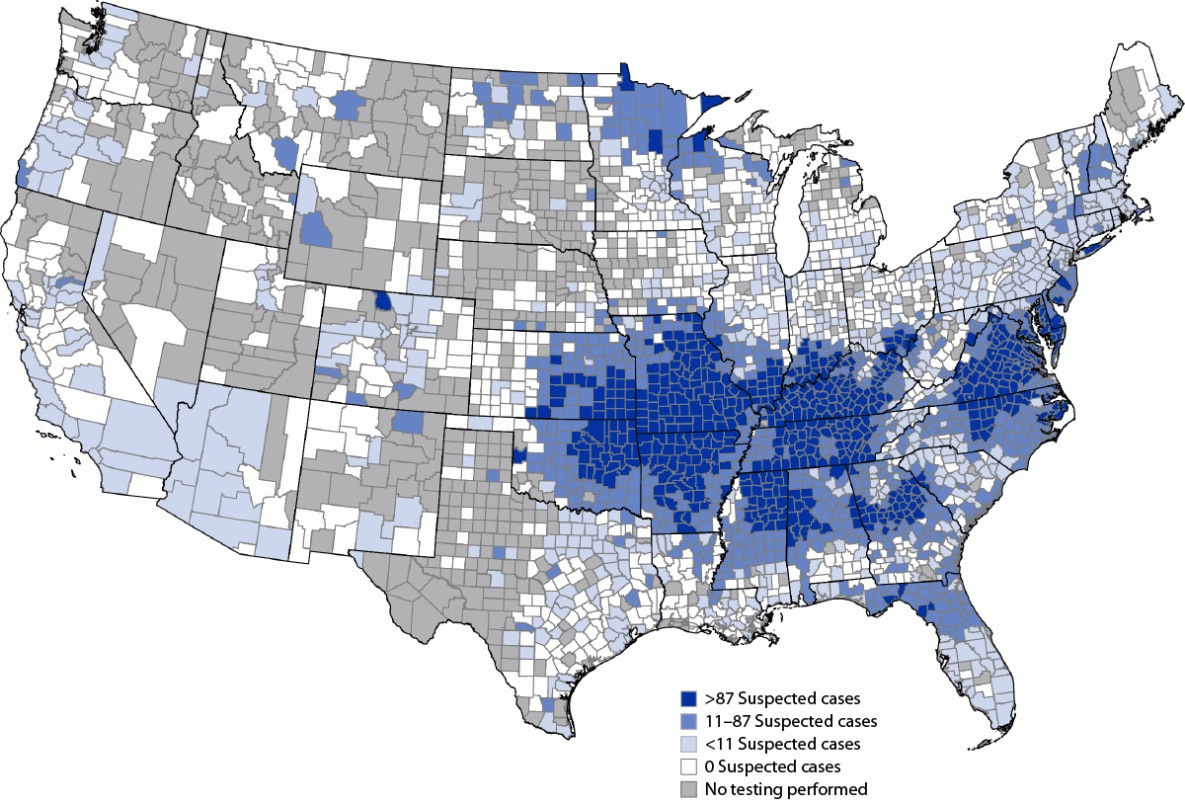
Abbreviations: IgE = immunoglobulin E; IU = international unit; kU = kilounit.
* A suspected case of alpha-gal syndrome was defined as being in a person who had confirmatory laboratory evidence (serum or plasma alpha-gal–specific IgE ≥0.1 IU/mL or ≥0.1 kU/L) with no clinical information available.
Figure: Geographic distribution of suspected alpha-gal syndrome cases per 1 million population per year in the U.S. from 2017-2022. Source: https://www.cdc.gov/mmwr/volumes/72/wr/mm7230a2.htm
Climate Change and Alpha-gal Syndrome
Climate change is one of several factors that affect when and where tickborne diseases and tick-associated conditions like AGS can occur. Increasing temperatures from climate change can influence tick life cycles by increasing a tick’s ability to reproduce, leading to larger tick populations and greater risk of disease transmission. Additionally, milder winters and warmer early spring temperatures expand the seasons when ticks are active, resulting in more weeks of the year that people in the U.S. are at risk of tick bites. Climate change can also impact the distribution and density of the wildlife ticks feed on (e.g., deer and small mammals) and, subsequently, lead to an expanded geographic distribution (e.g., latitude, altitude) of the diseases and conditions associated with these ticks. Expanding tick ranges and increasing disease incidence are also linked to changes in land use patterns, such as reforestation, forest fragmentation, and suburban development, which can lead to increased opportunities for humans to be exposed to ticks.
The best way to prevent AGS is to protect yourself from tick bites. If you have AGS, new tick bites may reactivate allergic reactions to products that contain alpha-gal, such as red meat. When outdoors, avoid grassy, brushy, and wooded areas where ticks may be found, and walk in the center of trails. Use EPA-registered insect repellents designated for protection from ticks and treat clothing and gear with 0.5% permethrin or buy pre-treated items. After time outside, check your clothing and gear for ticks; perform a thorough tick check on yourself, pets, and children; and take a shower. If you see an attached tick, remove it immediately.
Resources to Reduce Health Risks Associated with Alpha-gal Syndrome
Visit CDC’s websites to find more information:
- Alpha-gal Syndrome: Learn about common symptoms, products that may contain alpha-gal, and prevention measures
- Fight the Bite: Prevent bites from both ticks and mosquitoes
- Avoiding Ticks: Take steps to avoid ticks on yourself, on your pets, and in your yard
- Tick Bite Data Tracker: Explore the new tick bite data tracker, which shows Emergency Department visits for tick bites on a weekly and regional basis to help the public know when they may be most at risk of tick bites and give healthcare providers and public health personnel timely data to improve tick bite prevention efforts
